Voiding dysfunction / Disorders of Urinary Track
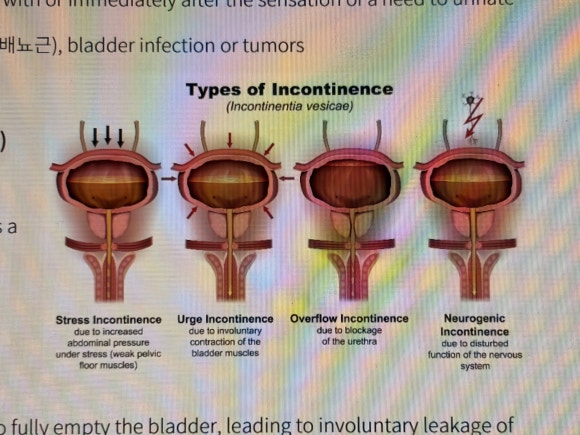
1. Incontinence(실금)
|
종류 |
설명 |
|
Stress |
|
|
Urge |
|
|
overflow |
|
|
Neurogenic |
|
|
Functional |
eg. Dementia, Immobility |
|
Enuresis |
|
|
Nursing interventions for incontinence |
|
|
|
2. Cystitis(UTI, 방광염)
|
Causes |
|
|
Predisposing factors |
Female(urethra), Increased age, Urinary catheter, DM, poor hygiene, urinary stasis |
|
Assessment(Manifestations, 증상) |
|
|
Nursing interventions |
|
👉 Antibiotic : sulfamethoxazole-trimethoprim (Bactrim) 👉 Urinary tract analgesics(진통제)/Antispasmoic(항경련제) : phenazopyridine
|
|
3. Urethritis(요도염)
-
Commoonly occures with a sexually transmitted infection(STI)
-
In man, mostly related to gonorrhea(임질) or chlamydial infection(클라미디아 감염증)
-
In women, caused by feminine hygiene spray or UTI
|
Assessment(Manifestations, 증상) |
|
|
Nursing interventions |
|
|
|
4. Pyelonephritis(신우신염)
-
An inflammation of the renal pelvis and the kidney tissue caused by bacterial infection
-
Usually occures when bacteria(E.Coli) from the bladder ascend to the kidneys, leading to infection
-
Chronic pyelonephritis can lead to AKI or CKD
|
Assessment |
|
|
Predisoposing factors |
|
|
Nursing interventions |
|
|
|
5. Glomerulonephritis(사구체신염)
👉 Commonly caused by group A beta hemolytic streptococcal infection
👉 Autoimmune disease(자가면역질환) |
|
|
Assessment(Manifestations, 증상) |
|
|
Nursing interventions |
|
|
|
|
Complications : Kidney failure, Pulmonary edema, Uncotrolled hypertension, Heart failure |
|
6. Nephrotic syndrome(신증후군)
|
Pathophysiology |
|
|
Assessment |
|
|
Dx |
24-hour urine for protein |
|
Med |
Corticosteroid therapy, Immunosuppressant therapy, diuretics |
|
Nursing interventions |
|
|
|
7. Renal calculi, Urinary catheter / Urinary diversion
|
Causes |
Hypercalcemia, dehydration, immobility, gout(통풍), increased intake of oxalate(spinach, peanuts, chocolate, avocado) |
|
Dx |
IV pyelogram(신우조영도), renal ultrasound, X-ray of KUB |
|
Assessment |
|
|
Nursing interventions |
|
|
Treatment |
Cystoscopy, ureteroscopy, ESWL, Percutaneous lithotripsy |
|
Surgery |
Ureterolithotomy, Pyelolithotomy, Nephrolithotomy, Nephrectomy |
출처 https://blog.naver.com/hips13/224258058678





 로그인을 해주세요
로그인을 해주세요